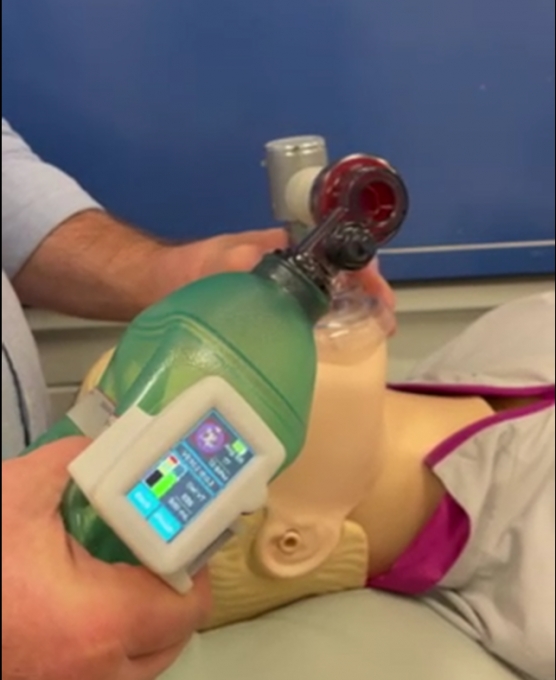
Ventilation management during life-saving resuscitation is being transformed by a local start-up, Abtulus®, who have partnered with the Medical Device Partnering Program (MDPP) at Flinders University to develop a novel Bag Valve Mask (BVM) guidance system.
Engineered by Dr Siavash Noor (Ahmadi Noorbakhsh) of Abtulus®, VentiWatch is a practical, simple and reusable ventilation management solution supporting medical professionals and first responders with the delivery of precise and efficient ventilation during resuscitation.
Read more

DeflectaCath tipped to redefine urological care.
An Australian clinical surgeon has collaborated with the Medical Device Partnering Program (MDPP) at Flinders University to develop a novel catheter for safely navigating the intricate curves and contours of the male urinary tract.
Urological surgeon Associate Professor Ian Middleton developed "DeflectaCath," a silicone catheter equipped with a unique deflection mechanism in its tip, to simplify the insertion procedure for clinicians and improve the health outcomes for patients.
Read more

Revolutionising the landscape of healthcare delivery, innovator Hayley Saddington has joined forces with Flinders University's Medical Device Partnering Program (MDPP) to build a cost-effective, clinically guided digital software application tailored for supporting in-home rehabilitation.
The co-founder of Peak Medical, Hayley is a visionary in her field who has exploited artificial intelligence to create an innovative technology which empowers in-home patients to progress their rehabilitation with the confidence of precise clinical guidance.
Replicating the physiotherapy experience, the technology employs an evidence-based clinical approach, directing individuals to customised exercises for continuous improvement between appointments.
Read more

Approximately 76,000 pregnant women and 500,000 babies die from pre-eclampsia across the world every year. Women in developing countries are seven times more likely to suffer from the condition due to delayed diagnosis and a lack of access to hospitals.
Causes of pre-eclampsia are not entirely understood, but if left untreated it can lead to blood clots, organ failure, and death. Rapid, affordable, and accurate diagnostic tools are therefore essential in aiding treatment.
Now, with the help of the Medical Device Partnering Program, a portable diagnostic device being developed by Professor Benjamin Thierry, Dr Duy Tran and a team from the University...
Read more

What started as a family injury has turned into a rehabilitation game-changer receiving global attention.
The Prohab Connected Healthcare Device, the brainchild of physiotherapist Lyndon Huf, is an innovative rehabilitation device that accurately measures the force-generating capability of an individual’s muscle, in order to guide and personalise prescription of exercise and rehabilitation programs .
Read more

When Orthopaedic Surgeon, Dr Matthew Liptak started noticing inconsistent outcomes in the rehabilitation of his patients after total knee replacement, he decided to take things into his own hands.
He identified a gap in the market for a simple and effective device to encourage, motivate and monitor the rehabilitation of his patients post-surgery.
Dr Liptak first approached the MDPP in 2013 for assistance with the development of Maxm Skate, a skate-like device which straps to a patient’s foot. Whilst he had an initial prototype of the skate, he needed R&D assistance to develop a sensor which would record the user’s range of...
Read more

Detecting cancer is set to become safer and more accurate with the development of a new cancer-detecting probe.
The probe, an invention of University of South Australia researchers Professor Benjamin Thierry and Dr Aidan Cousins, provides a non-radioactive alternative to map how cancer has disseminated through the body.
Following initial bench-top testing of the device, the team first partnered with the MDPP in 2013, seeking out electronic engineering expertise and advice from end users and commercial experts.
Read more

Since 1987, world-renowned sleep psychologists, Professor Leon Lack and Dr Helen Wright from Flinders University, have studied the effects of light on the human body clock.
Their work focused on circadian rhythms, the fluctuations in biological process occurring on a 24-hour basis in the body. Research determined that exposure to bright light can normalize the timing of the rhythms and assist with the treatment of insomnia, winter depression, jet-lag and shift work disorder.
The result of this extensive body of work was Re-Timer, glasses proven to re-time one’s body clock. The glasses shine glowing green-blue light into the eye of the wearer...
Read more

When Professor Matthew McDonald and Dr Peter Pedoulias had a revelation in the operating theatre about how spinal fusion surgery could be improved they turned to the Medical Device Partnering Program to make it a reality. Spinal fusion is a surgical procedure that corrects issues of the small bones of the spine by permanently connecting two or more vertebrae. This complex surgery is often the last resort to treat back problems and can cost around $46,700 per patient.
Read more























